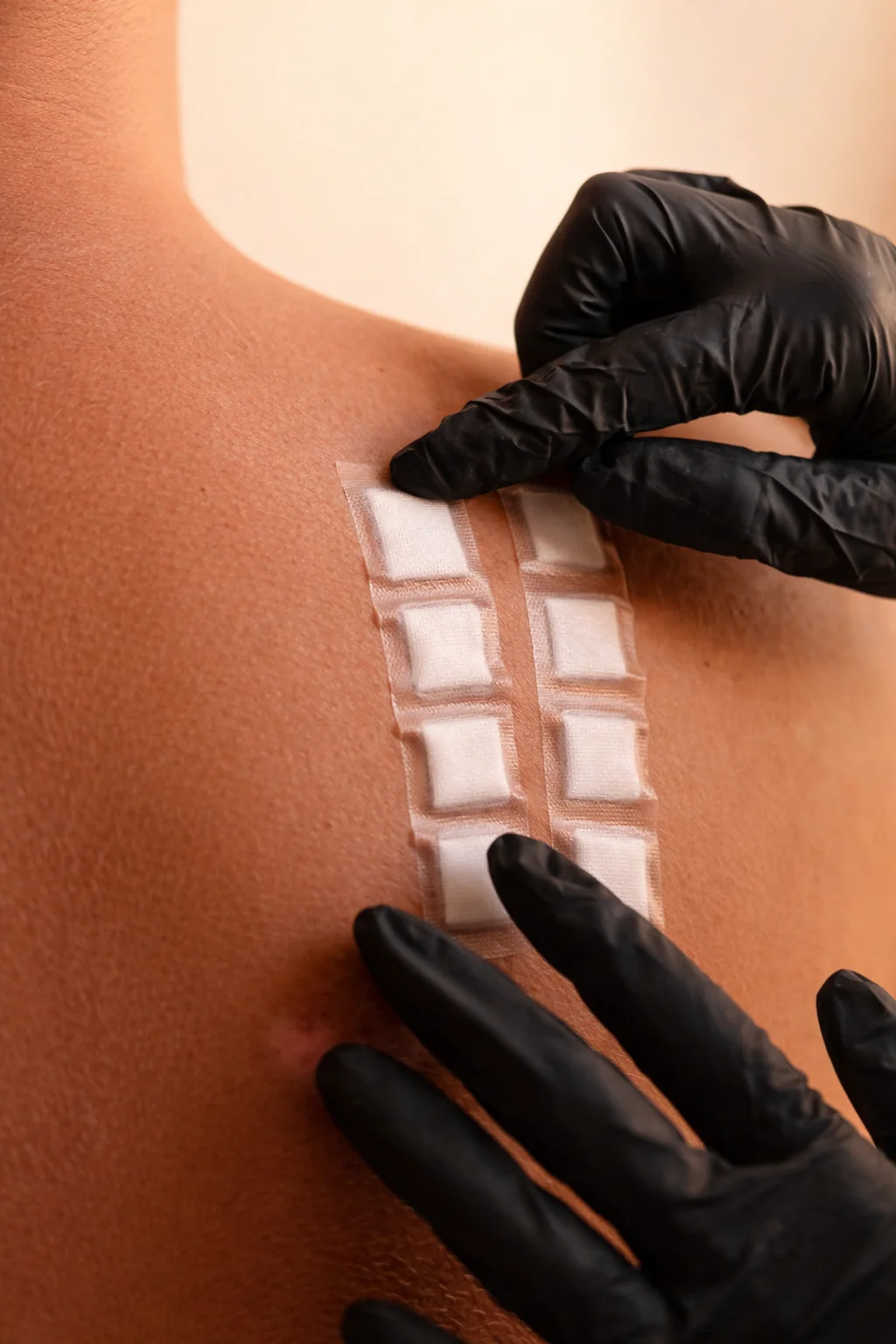
Patch Testing

Patch Testing Treatment
Patch Testing Treatment Statistics and Key Information
- Patient Satisfaction Rate
- 95%
- Average Treatment Cost
- See provider pricing
- Number of Reviews
- 10065
- Treatment Downtime Duration
- Varies by treatment
- Number of Available Practitioners
- 295
Overview
Patch testing is a **diagnostic skin allergy test** that helps figure out whether specific substances that touch your skin are causing allergic reactions like contact dermatitis or eczema. Tiny amounts of known potential allergens (like nickel, fragrances, preservatives or rubber chemicals) are applied on small patches and fixed onto your back or upper arms. You wear them for about 48 hours, then the dermatologist removes them and checks for reactions (redness, itch, swelling) usually again a couple of days later because delayed allergic responses take time to show up. It’s not like a prick test for immediate hay fever — it’s about delayed, contact triggers.
Goals of Patch Testing treatment
- Identify which specific substances (allergens) may be triggering your skin rash or dermatitis.
- Distinguish allergic contact dermatitis from irritant dermatitis or other skin conditions.
- Help you avoid substances that flare up your skin and guide personalised management.
- Support a care plan (topical treatments, avoidance strategies) based on concrete test results.
Treatment Options
- Patch testing is diagnostic, not therapeutic — it finds the *cause* rather than *treat the rash* directly.
- Unlike skin prick tests or blood IgE tests, patch tests specifically look for delayed contact reactions, so they’re complementary tools, not direct alternatives.
- At-home elimination protocols (switching soaps, gloves etc) can give clues but aren’t as systematic as patch testing panels.
- Topical treatment without testing might suppress symptoms but not tell you what’s actually triggering them.
Pros
- Can pinpoint the *actual cause* of persistent or recurrent dermatitis when history alone isn’t clear.
- Helps reduce unnecessary trial-and-error avoidance of products and exposures.
- Low risk for most people and gives actionable avoidance guidance.
- Useful in occupational skin disease, where repeated exposures at work matter.
Cons
- You need multiple visits over a few days to complete the test and readings.
- Results can be a bit uncomfortable if you react (redness, itch, sometimes blistering).
- It doesn’t test for inhaled or food allergies (so it’s limited to contact triggers).
- Interpreting results well requires real clinical skill, otherwise you can over- or under-read reactions.
Candidate & Preparation
Who is a Good Candidate
- Someone with **persistent or recurrent dermatitis/eczema** and suspected contact allergy.
- People with unexplained rashes that come and go with exposures.
- Individuals with occupational exposures to chemicals/materials that could irritate skin.
- Children and adults alike can be candidates, but some cases (widespread rash on test site, recent sunburn) may delay or complicate testing.
Appointments & Safety
What Happens During Appointment
Usually three visits over about a week: on Day 1 you have the consultation and patches applied (tiny allergens on adhesive chambers), on Day 2 (~48 hours) the early reading happens when patches are removed, and on Day 4–5 another reading captures delayed reactions. Each visit can be ~20–60 minutes depending on discussion and readings.
Pain Level
It’s usually *not painful* like an injection — most people feel only mild irritation or itch where patches react.
Safety Considerations
- Patch testing is generally safe and minimally invasive, but **mild itch, redness or burning** at test sites is common.
- Strong reactions can cause blisters or temporary pigmentation changes — usually not serious but monitored.
- Rarely, a severe reaction can happen, so it’s done in clinics prepared to manage flare-ups.
Cost & Access
Typical Prices
Private patch testing can vary a lot. For example, consultant-led packages in London might quote around **GBP 600 for the full test** including application and readings, on top of a **consultation fee (e.g. GBP 250)**. Some other clinics break it down (application ~GBP 200, review ~GBP 160 etc). These are just examples — remote or NHS testing is generally free at point of care on the NHS.
Why Prices Vary
- Whether the test includes **all appointments, readings and a written avoidance plan** or only the application.
- Experience and qualifications of the clinician (consultant dermatologist vs general clinic).
- Location (central city clinics are usually pricier).
- Number and type of allergen panels used or any expanded/custom panels.
Results & Maintenance
How Long Results Last
The **results themselves are instant** once interpreted — you know which substances you reacted to at the final reading. What *lasts* is the avoidance knowledge: if you avoid allergens identified, you can prevent future flares. Avoidance is ongoing, because contact allergies usually stay once you’re sensitised.
Maintenance Requirements
- You usually get one structured series of tests with readings in a week. If new exposures arise later, your clinician might repeat or expand testing.
- Avoidance guidance from the first test is ongoing; if new symptoms show, a re-assessment can happen years later.
Regulation & Guidelines
Guidelines
There isn’t a single NICE guideline focused only on patch testing, but NICE guidance on dermatitis and allergy includes when to investigate with patch testing. NHS dermatology services commonly use internationally recognised patch test series under standards like the British Dermatological Nursing Group and UK practice guidance. MHRA doesn’t specifically regulate patch testing as a device but governs safety standards of allergen materials and clinical diagnostics.
What to Do If Something Goes Wrong
Regulation
Patch testing is a **clinical diagnostic procedure** usually done by dermatologists in NHS or private clinics and falls under general healthcare standards and professional regulation (GMC etc). There isn’t a unique UK guideline just for patch testing, but dermatology practice follows evidence and safety standards.
Complaints
If you have a bad experience, raise it with the clinic’s complaints process or professional regulator (eg GMC for doctors), and local authority standards for clinical procedures.

